The Rise of Remote Care and Assistive Technology
Healthcare is undergoing one of the largest digital transformations in history. Advances in Internet of Things (IoT) technologies, artificial intelligence, wearable sensors, and telehealth platforms are fundamentally changing how care is delivered.
Rather than requiring patients to visit hospitals or clinics for routine monitoring, healthcare providers increasingly rely on remote patient monitoring (RPM) and connected medical devices that continuously collect and transmit patient data.
These technologies are particularly transformative for:
- Aging populations
- People with chronic illnesses
- Individuals with disabilities
- Patients living in rural or underserved areas
The ability to monitor health conditions remotely has enormous benefits. It enables early intervention, reduces hospital admissions, lowers healthcare costs, and allows individuals to live independently while maintaining continuous medical oversight.
However, one critical component is often overlooked in discussions about digital healthcare transformation:
Connectivity.
Every remote monitoring device, wearable medical sensor, emergency alert system, or assistive technology platform depends on reliable connectivity to transmit life-critical data.
Without reliable connectivity, the entire remote care ecosystem fails.
This article explores the rapidly expanding remote care and disability technology market, the connectivity challenges that threaten its effectiveness, and how multi-carrier IoT connectivity solutions, such as Multi-IMSI and eSIM technology, are solving these challenges.
We will also explore how connectivity platforms such as Fidelitel Solutions play a critical role in ensuring always-on connectivity for healthcare IoT devices.
The Global IoT Healthcare Market
The healthcare sector is becoming one of the largest adopters of IoT technologies.
Industry analysts estimate that the global IoT healthcare market will grow dramatically over the next decade.
Current projections suggest:
- 2024–2025 market size: approximately $56–$65 billion
- 2034–2035 projected size: $368–$594 billion
This represents one of the fastest-growing sectors in the global IoT ecosystem.
Several major factors are driving this growth.
1. Aging Global Population
The global population is aging rapidly.
By 2050, the number of people aged 65 and older is expected to exceed 1.6 billion worldwide.
Older populations require:
- Continuous monitoring
- Chronic disease management
- fall detection
- medication tracking
- emergency response systems
IoT-enabled monitoring devices provide these capabilities while allowing individuals to remain in their homes.
2. Rising Healthcare Costs
Healthcare systems worldwide are under intense financial pressure.
Remote care technologies help reduce costs by:
- preventing hospital readmissions
- enabling early diagnosis
- reducing emergency visits
- minimizing inpatient stays
Studies show that remote patient monitoring programs can reduce hospital readmissions by up to 50%.
Increased Adoption of Telehealth
Telehealth adoption surged dramatically during the COVID-19 pandemic.
Even after the pandemic, telehealth usage remains far higher than pre-2020 levels.
Healthcare providers increasingly use telehealth platforms for:
- follow-up visits
- chronic disease management
- mental health consultations
- specialist care access
However, telehealth is only effective when stable connectivity exists.
Advancements in Sensor Technology
Modern medical devices now include sophisticated sensors capable of measuring:
- heart rate
- blood pressure
- oxygen saturation
- glucose levels
- body temperature
- sleep quality
- physical activity
These sensors continuously generate data that must be transmitted to healthcare providers.
Connectivity reliability becomes essential.
Remote Patient Monitoring (RPM): The Backbone of Digital Healthcare
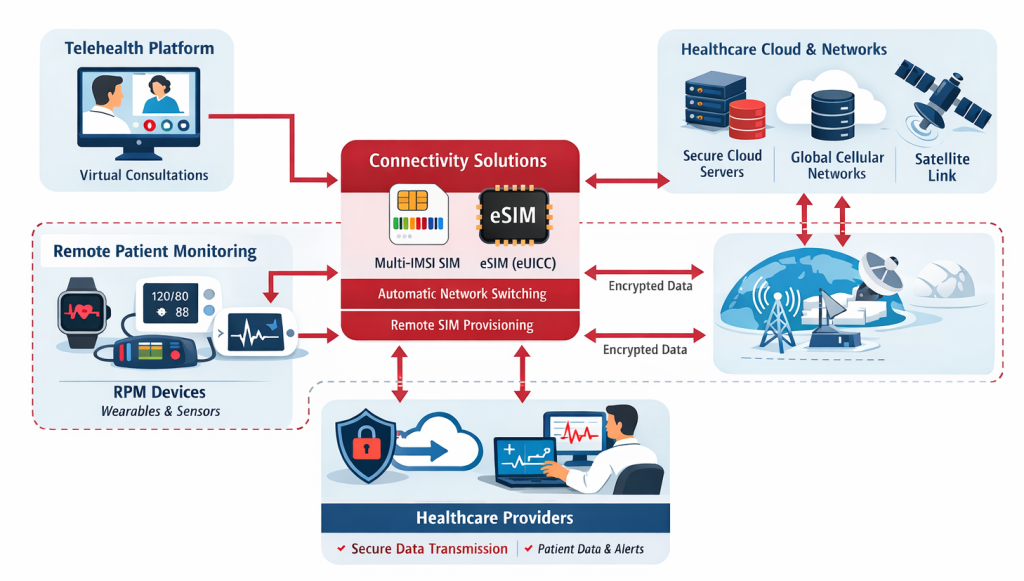
Remote Patient Monitoring (RPM) is the largest and most rapidly expanding segment of the IoT healthcare market.
RPM uses connected devices to continuously collect patient health data and transmit it to healthcare providers for monitoring and analysis.
Common RPM devices include:
- wearable heart monitors
- connected blood pressure cuffs
- glucose monitors
- pulse oximeters
- ECG patches
- smart inhalers
- medication adherence trackers
By 2024, more than 60 million Americans were already using some form of remote patient monitoring.
RPM provides significant clinical benefits.
Reduced Hospital Readmissions
Continuous monitoring allows providers to detect early warning signs of deterioration.
This enables early intervention before conditions become severe.
Studies show RPM programs can reduce hospital readmissions by 30–50%.
Better Chronic Disease Management
Chronic diseases such as:
- diabetes
- hypertension
- heart disease
- COPD
require continuous monitoring.
RPM allows physicians to track patients daily rather than only during occasional clinic visits.
Improved Patient Engagement
Patients who monitor their own health metrics often become more engaged in their treatment plans.
This improves adherence to medication and lifestyle recommendations.
Aging in Place and Independent Living
Another major driver of remote care technology adoption is the concept of aging in place.
Many seniors prefer to remain in their homes rather than move into assisted living facilities.
IoT-enabled technologies help make this possible.
Smart homes equipped with sensors can monitor:
- movement patterns
- sleep behavior
- medication usage
- appliance usage
- fall detection
If unusual patterns occur, caregivers or healthcare providers can be alerted.
Examples of aging-in-place technologies include:
- fall detection sensors
- motion detectors
- smart medication dispensers
- connected emergency alert buttons
- health monitoring wearables
However, these devices are only effective if they maintain continuous connectivity.
A device that cannot transmit alerts is essentially useless.
Assistive Technologies for People with Disabilities
Assistive technologies are another rapidly growing segment of the IoT healthcare market.
Globally, more than 2.5 billion people require assistive products.
These technologies help individuals with disabilities maintain independence and mobility.
Examples include:
Smart Wheelchairs
Advanced wheelchairs now include:
- obstacle detection
- navigation assistance
- GPS tracking
- remote diagnostics
Wearable Navigation Devices
Devices designed for visually impaired individuals can provide:
- real-time navigation
- obstacle alerts
- voice guidance
Speech-to-Text and Communication Devices
For individuals with speech impairments, assistive devices convert speech to text or enable alternative communication methods.
Medical Alert Systems
Emergency alert systems allow users to call for help during medical emergencies.
These systems often rely on cellular connectivity.
If connectivity fails, emergency assistance cannot be triggered.
Why Connectivity Is the Hidden Backbone of Remote Care
While healthcare IoT devices receive significant attention, the connectivity infrastructure powering these devices often receives far less attention.
However, connectivity is the most critical component of remote care systems.
Without reliable connectivity:
- vital signs cannot be transmitted
- emergency alerts cannot be sent
- telehealth calls fail
- monitoring dashboards receive incomplete data
This can result in delayed care or life-threatening situations.
Most connected healthcare devices rely on one of the following connectivity options:
- Wi-Fi
- Cellular networks
- Bluetooth connections to smartphones
- Ethernet connections
- Satellite connectivity in remote areas
However, many devices rely primarily on cellular networks for reliability and mobility.
Unfortunately, many healthcare devices are designed with single-carrier connectivity, which introduces major risks.
The Critical Risks of Single-Carrier Connectivity
Devices that rely on a single cellular carrier face several critical risks.
Single Point of Failure
If the network experiences an outage, the device becomes completely disconnected.
This is unacceptable for life-critical medical devices.
Weak Signal Coverage
Signal strength varies significantly by location.
A single carrier may have strong coverage in one area but weak coverage nearby.
Poor Indoor Penetration
Signals can be blocked by:
- concrete walls
- steel structures
- energy-efficient windows
This can cause connectivity failures inside buildings.
Rural Connectivity Gaps
Many rural areas have limited cellular coverage.
A device locked to one network may lose connectivity completely.
The Real-World Consequences of Connectivity Failure
Connectivity failures can have severe consequences in healthcare environments.
These include:
- Loss of Vital Monitoring Data: If monitoring data stops transmitting, physicians lose visibility into patient health.
- Delayed Emergency Alerts: Emergency alert devices may fail to notify caregivers.
- Increased Anxiety for Patients: Patients may lose confidence in remote care technologies if connectivity fails.
- Increased Workload for Caregivers: Care teams must spend time troubleshooting devices rather than providing care.
Multi-IMSI Technology Explained
Multi-IMSI technology addresses these connectivity challenges by allowing a single SIM card to store multiple carrier identities.
IMSI stands for International Mobile Subscriber Identity.
A traditional SIM contains only one IMSI tied to a single network operator.
A Multi-IMSI SIM contains several IMSI profiles from different operators.
This allows the device to automatically switch between networks.
Benefits include:
- improved signal coverage
- network redundancy
- automatic failover
If one network becomes unavailable, the device switches to another carrier.
eSIM and eUICC Technology Explained
An eSIM (embedded SIM) is a programmable SIM chip embedded directly into a device.
Unlike traditional SIM cards, eSIMs can be remotely programmed.
The technology that enables this is called eUICC (Embedded Universal Integrated Circuit Card).
With eUICC, network operator profiles can be downloaded over the air.
Benefits include:
- remote provisioning
- remote carrier switching
- simplified device management
Multi-IMSI vs eSIM: What Is the Difference?
These technologies are often confused.
Multi-IMSI
- multiple IMSI identities stored on SIM
- automatic switching between carriers
eSIM / eUICC
- programmable SIM chip
- remote profile downloads
The two technologies can also be combined.
Why Multi-IMSI + eSIM Is the Ultimate Connectivity Solution
Combining Multi-IMSI with eSIM provides maximum connectivity flexibility.
Devices can:
- switch between preloaded carrier profiles
- download new profiles remotely
- maintain connectivity globally
This creates always-on connectivity.
The Role of 5G in Remote Healthcare
5G networks bring significant improvements to healthcare connectivity.
Benefits include:
- ultra-low latency
- high bandwidth
- support for massive IoT deployments
This enables real-time applications such as:
- remote surgery support
- high-resolution telemedicine video
- continuous monitoring of large patient populations.
Security Challenges in Connected Healthcare
Healthcare data is extremely sensitive.
Connected devices must comply with strict regulations such as:
- HIPAA
- GDPR
- regional healthcare privacy laws
Multi-carrier connectivity platforms must implement strong security controls.
Connectivity Architecture for Medical IoT Devices
A typical remote care architecture includes:
- Medical device sensors
- Connectivity module (cellular modem)
- SIM or eSIM profile
- IoT connectivity platform
- Cloud healthcare platform
- clinical monitoring dashboards
Connectivity reliability is essential at every stage.
The Role of Connectivity Platforms
Connectivity platforms manage:
- SIM provisioning
- network switching
- device monitoring
- usage analytics
- security policies
This is where platforms like Fidelitel Solutions play a crucial role.
How Fidelitel Solutions Enables Reliable Healthcare Connectivity
Fidelitel Solutions provides a multi-carrier IoT connectivity platform designed for mission-critical applications.
Key capabilities include:
- Multi-Carrier Connectivity: Devices can connect to multiple cellular networks, ensuring the strongest available signal.
- Multi-IMSI SIM Technology: SIMs automatically switch between carriers to maintain connectivity.
- eSIM / eUICC Support: Devices can receive new operator profiles remotely.
- Global Coverage: Devices can operate internationally without complex roaming restrictions.
- Connectivity Management Platform: Organizations can monitor devices, manage SIM profiles, and analyze connectivity performance.
- Managed Connectivity Services: Fidelitel provides managed services that monitor device connectivity and prevent downtime.
Best Practices for Deploying Remote Care Devices
Healthcare organizations should implement several best practices.
- Redundancy Planning: Devices should support multi-carrier connectivity.
- Connectivity Monitoring: Organizations should monitor device connectivity in real time.
- OTA Updates: Devices should support remote updates.
- Security Controls: Encryption and authentication must be implemented.
The Future of Remote Care Connectivity
The future of remote healthcare will be shaped by several technologies:
- AI-driven predictive analytics
- 5G and future 6G networks
- edge computing
- satellite IoT connectivity
- global multi-carrier networks
Connectivity platforms will play a central role.
Conclusion: Building a Resilient Remote Care Ecosystem
Remote care technologies are transforming healthcare delivery worldwide.
However, the effectiveness of these systems depends entirely on reliable connectivity.
Single-carrier connectivity introduces unacceptable risks for healthcare IoT devices.
Technologies such as Multi-IMSI and eSIM provide the redundancy and flexibility required for mission-critical medical applications.
By combining these technologies with advanced connectivity platforms such as Fidelitel Solutions, healthcare providers and device manufacturers can ensure always-on connectivity for remote care systems.
As the global IoT healthcare market approaches hundreds of billions of dollars, organizations that invest in resilient connectivity infrastructure will lead the next generation of digital healthcare innovation.